By Curt Squires
When it comes to a stroke, time is critical. The longer a stroke remains untreated, the more damage that is done.
“Time is brain,” said Charles Rosen, MD, Ph.D., a neurosurgeon with OSF HealthCare Illinois Neurological Institute in Bloomington. “Unfortunately, what happens is people will say, ‘Oh, I don’t need to go. It’ll get better overnight.’ That can be dangerous because there is a small window of opportunity that needs to be exploited when symptoms occur.”
Those symptoms are easy to remember with the acronym B.E. F.A.S.T.
B – Balance lost
E – Eyes blurry
F – Facial drooping
A – Arm weakness or numbness
S – Speech difficulty or slurring speech
T – Time to call 9-1-1
Ignoring these symptoms can be a bad idea for two reasons, Dr. Rosen continued. It makes them more likely to become permanent. And second, they are often harboring something more serious that’s about to occur. After all, if you smell smoke in your house, it’s not a good idea to go to sleep and see if it’s better in the morning.
Certified Stroke Center
Since 2007, OSF HealthCare St. Joseph Medical Center has earned the Gold Seal of Approval from the Joint Commission. This means OSF St. Joseph is a certified stroke center, a rare distinction for hospitals providing neuroscience care.
Because “time is brain,” OSF St. Joseph has a defined stroke process to deliver the best possible care in a timely manner, said Ajeet D. Gordhan, MD, a neuroradiologist with OSF St. Joseph.
A critical part of the first step is imaging with computed tomography, commonly called a CT. Protocols around what the imaging shows and the outcome of the patient’s exam inform the care team what to do next. Usually strokes are divided into two categories: hemorrhagic stroke which is a bleeding into the brain, or ischemic stroke, where a blood vessel is obstructed.
A CT is a fair indicator as to what the next steps would be, Dr. Gordhan continued. So if it is negative for a bleed, then the first consideration is usually to begin intravenous tissue plasminogen activator (TPA), which is a standard of care. TPA is an effective clot-busting drug that works to dissolve a clot in the brain to improve blood flow that is being deprived from the clot, causing the stroke.
Technology
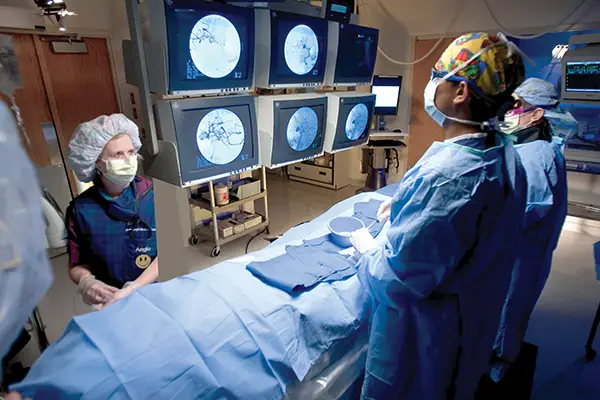
The OSF St. Joseph catheterization angiography (angio) lab was upgraded in June and is where OSF St. Joseph really shines and allows us to be at forefront of neuro-endovascular care, said Dr. Gordhan.
The angio lab is basically an operating room with state-of-the-art equipment used in treating a clot in the brain, he continued. The lab has the most advanced ancillary imaging that allows multiple things to be done including blood perfusion and flow imaging, and CT’s right on the table.
“It’s like having the most expensive iPad in the world,” Dr. Gordhan explained. “And what this iPad does for you, it allows us to see through blood vessels as we navigate these devices into the vessel that is affected.”
“The rationale is that we want to reestablish blood flow as fast as possible. And now we have five or six randomized controlled trials that prove its efficacy. It’s probably the best way of giving a patient a larger vessel occlusion and a favorable outcome.”
If the patient presents with a bleed, OSF St. Joseph has the tools required to ensure they are safely and adequately treated for their condition.
“Some bleeds need to be treated regardless but the source of the bleed is an important part of the equation,” said Dr. Rosen. “Sometimes that needs to be addressed through the endovascular techniques that Dr. Gordhan has alluded to. Sometimes they need to be addressed surgically. Sometimes we’ve even done some sort of combination therapy.”
Teamwork
“I think what is special, is Dr. Gordhan and I have clinic together,” said Dr. Rosen. “So a patient comes to see one of us, and it’s very easy for us to involve the other one. So it is very common for one of us to see a patient and walk three feet down the hall and say, ‘Hey, let me show you this. What do you think?’”
It’s really nice having this collaboration where the goal is what is in the patient’s best interest in implementing a care plan to get the best possible care.
“And I think that’s really special and uncommon in a lot of medical centers, where oftentimes egos can get in the way,” explained Dr. Rosen. “Ajeet and I have a special relationship where we don’t have that issue. We talk about and try to find what’s best for the patient so that the patient gets the best possible care.”
Dr. Gordhan said his colleague is in a very small community of folks that meddle with the brain and blood vessels. “And as the only surgeon in Bloomington who manages vascular issues of the brain, he gives us the ability and opportunity to treat issues that we think are feasible and safe.”
Don’t wait to be seen
The majority of people who hesitate to come in for care, think it is something minor and will get better in the morning or think they will be embarrassed if we don’t find anything, Dr. Rosen said.
“The other thing I would say is that sometimes people have symptoms that they think are strokes, and they come here and it turns out they have something else. What’s nice is we have the ability to deal with all brain lesions here, so they should have a low filter for seeking care when it comes to the development of a new deficit. That is not something to wait to see if it gets better.”
Learn your stroke risk assessment at osfhealthcare.org/assessments.